Canine immune-mediated polyarthritis
Myles McKenna MVB MVetSci MVetMed DACVIM (SAIM) DECVIM-CA MRCVS, assistant professor in small animal internal medicine at University College Dublin, presents an overview of canine immune-mediated polyarthritis
Canine immune-mediated polyarthritis (IMPA) is a common but under-recognised condition in clinical practice. IMPA is characterised by synovitis of two or more joints, which is responsive to immunosuppressive therapy.1 It is often associated with systemic signs of illness such as pyrexia, lethargy and hyporexia.2,3 Most affected dogs are between three and seven years of age at the time of diagnosis, although cases of IMPA have been reported in dogs ranging from six months to 12 years of age.2,4 Any breed can be affected and there is no apparent sex predilection.1,2,4
Pathophysiology
IMPA can be classified as erosive, where progressive joint destruction occurs, or non-erosive. Non-erosive IMPA typically results from a type III hypersensitivity reaction, involving the deposition of immune complexes in the synovial basement membrane in response to an immune stimulus. This starts a cascade reaction that draws inflammatory cells, including neutrophils, to the site of inflammation.5 Erosive IMPA most commonly occurs when plasma cells or activated B cells produce a pathogenic immunoglobulin called rheumatoid factor.1 Circulating rheumatoid factor is deposited and phagocytosed in the synovium, leading the release of inflammatory mediators and the activation of osteoclasts. Osteoclast activation leads to subchondral bone resorption, while fibroblast proliferation leads to scarring and deformation of joints. Erosive disease is rare, representing less than 1% of cases of IMPA.1,2,6
Classification of IMPA
In addition to being classified as erosive or non-erosive, IMPA may be classified as primary (idiopathic), or secondary (where IMPA is triggered by a distant immunogenic stimulus).1 Most cases of IMPA are primary, or idiopathic, meaning no underlying cause is identified.1,4,7 Primary IMPA is a diagnosis of exclusion; ruling out all possible causes of secondary IMPA is necessary before a diagnosis of primary IMPA can be reached. Causes of secondary IMPA include:
Infection: infection distant to the joint may serve as a source of excess antigens contributing to the development of immune complexes. Multiple sites and types of infection have been linked to IMPA including urinary tract infection, respiratory tract infection, endocarditis, borreliosis and leishmaniosis.1,4,8
Neoplasia: neoplastic cells may act as a source of persistent antigen, leading to secondary IMPA. Various types of neoplasia have been associated with secondary IMPA, including mammary carcinoma, squamous cell carcinoma and seminoma.1,4,9
Chronic gastrointestinal disease: including inflammatory bowel disease.1
Medications: IMPA is a rarely reported adverse effect of certain medications, most notably antibiotics. Sulfonamides are most commonly implicated, but other medications that have been linked to IMPA include penicillin derivatives, cephalosporins and phenobarbital.10-13
Vaccination: the immune stimulation induced by vaccination may represent a trigger for IMPA, and vaccines have been implicated as inciting causes of IMPA.14,15 However, there is a paucity of cases of vaccine-induced IMPA reported in the veterinary literature and a direct causal link is challenging to prove.
Occasionally, IMPA may be present not as a standalone immune-mediated disorder, but may instead be part of a polysystemic immune-mediated disorder such as systemic lupus erythematosus (SLE).16-18 In such cases, additional clinical manifestations such as haemolytic anaemia, thrombocytopenia, skin lesions or glomerulonephritis may be noted. Breed-associated IMPA has also been recognised, affecting breeds including the Japanese Akita, Shar Pei and Beagle.19-23 The Shar Pei IMPA syndrome, commonly termed ‘familial Shar-Pei fever’, is a distinct pathogenic process, representing a form of familial amyloidosis that is characterised by recurrent bouts of fever and joint inflammation, especially of the tarsi.20-23 In addition, a specific form of erosive arthritis has been reported in greyhounds.6,24,25
Clinical presentation
Typical clinical signs of IMPA include reluctance to walk and a shifting lameness, and multiple effused joints are usually (but not always) palpable on physical examination.1,2,7 Affected joints are commonly painful, but in one study only 40% of IMPA cases had joint pain detected on physical examination.2 The carpal and tarsal joints are more commonly affected than the larger and more proximal joints of the limbs.1,4 Other non-specific signs of illness such as weight loss and anorexia are variably present.2,3,4 Approximately half of affected patients are pyrexic on presentation. Because not all patients with IMPA will present with signs of overt lameness or joint effusion, it should always be considered as a differential diagnosis in dogs with non-specific clinical signs like pyrexia or lethargy.26
Diagnostic investigations
Although the diagnosis of IMPA is made by interpretation of synovial fluid cytology, dogs with suspected or confirmed IMPA require extensive diagnostic investigations to rule out other causes of polyarthropathy such as septic arthritis or osteoarthritis, to screen for erosive disease, and to rule out underlying infectious or neoplastic triggers of IMPA.
Baseline diagnostics
Complete blood count, serum biochemistry, urinalysis and urine culture should be performed in all cases. It is common to identify changes consistent with systemic inflammation on blood tests, such as leukocytosis, non-regenerative anaemia, and hypoalbuminemia.1,4 Mildly increased ALP of unknown aetiology is another commonly identified abnormality.4 A 4Dx SNAP test should routinely be performed to screen for vector-borne infections (Borrelia burgdorferi, Anaplasma spp., Ehrlichia spp. and Dirofilaria immitis). Additionally, quantitative Leishmania serology is recommended if dogs have a history of travel from areas of continental Europe where this parasite is endemic.
Imaging
Thoracic and abdominal imaging should be performed in all cases of suspected IMPA. Thoracic radiography and abdominal ultrasound, or alternatively thoracic and abdominal computed tomography (CT) are commonly performed. At least two peripheral joints should also be imaged via radiography or CT, to screen for the presence of erosive disease and rule out other joint pathology. Intracapsular swelling, indicating effusion, is detected in most dogs with non-erosive IMPA. In erosive IMPA, additional abnormalities including subchondral bone erosion, luxations or ankylosis may be present.27 In early erosive disease, no radiographic lesions may be present,28 therefore repeating radiographs of affected joints should be considered in dogs who fail to respond to treatment as expected, or who experience relapse of their disease.
Arthrocentesis
Arthrocentesis should be performed in all cases where IMPA is suspected, even if joint effusion is not present on physical examination. It may be performed early in the diagnostic process, or after the aforementioned baseline tests have been performed. Arthrocentesis should only be performed under deep sedation or general anaesthesia. Sampling a minimum of three joints is suggested to maximise the chance of obtaining a diagnosis. Because smaller peripheral joints are most commonly affected, sampling the tarsi and carpi should be prioritised.1,4 Sterile preparation of the areas to be sampled is essential to minimise the chance of iatrogenic septic arthritis. A 23-gauge or 25-gauge needle should be used, and the minimum volume of synovial fluid necessary collected, to decrease the risk of iatrogenic blood contamination of samples. Synovial fluid should be collected in an ethylenediaminetetraacetic acid (EDTA) tube for cytology and a plain tube for bacterial culture and sensitivity, and smears should be made immediately because synovial fluid cells commonly undergo rapid degradation in tubes. Normal synovial fluid should be clear and viscous.1 On cytology, normal joint fluid has a low nucleated cell count (<3000 cells/µL) and a protein concentration <2.5g/dL.29 Mononuclear cells are the predominant cell type. Synovial fluid of dogs with IMPA is often grossly turbid and less viscous. Nucleated cell count is >3,000 cells/µL, protein concentration is >2.5g/dL and on cytology non-degenerate neutrophils are usually the predominant cell type (see Figure 1). Dogs who have already received immunosuppressive medications or have more chronic disease may have a lower percentage of non-degenerate neutrophils in their synovial fluid, but a differential cell count comprising of >12% non-degenerate neutrophils is still considered consistent with IMPA.1,29 The presence of degenerate neutrophils and intracellular bacteria in synovial fluid is consistent with septic arthritis. However, it is important to note that non-degenerate neutrophils and no bacteria may be seen on cytology of joint fluid in some cases of septic arthritis, mimicking IMPA. Bacterial culture of joint fluid should always be performed in conjunction with cytology, although culture is positive in only 40-50% of septic joints.7,29,30 Differentiating IMPA from septic arthritis therefore requires thorough assessment of a dog’s history, physical examination findings and results of other diagnostic tests. Septic arthritis more commonly affects one large joint, whereas it is unusual for septic arthritis to manifest as a polyarthropathy affecting multiple smaller joints (although this is possible if haematogenous spread of infection has occurred).1
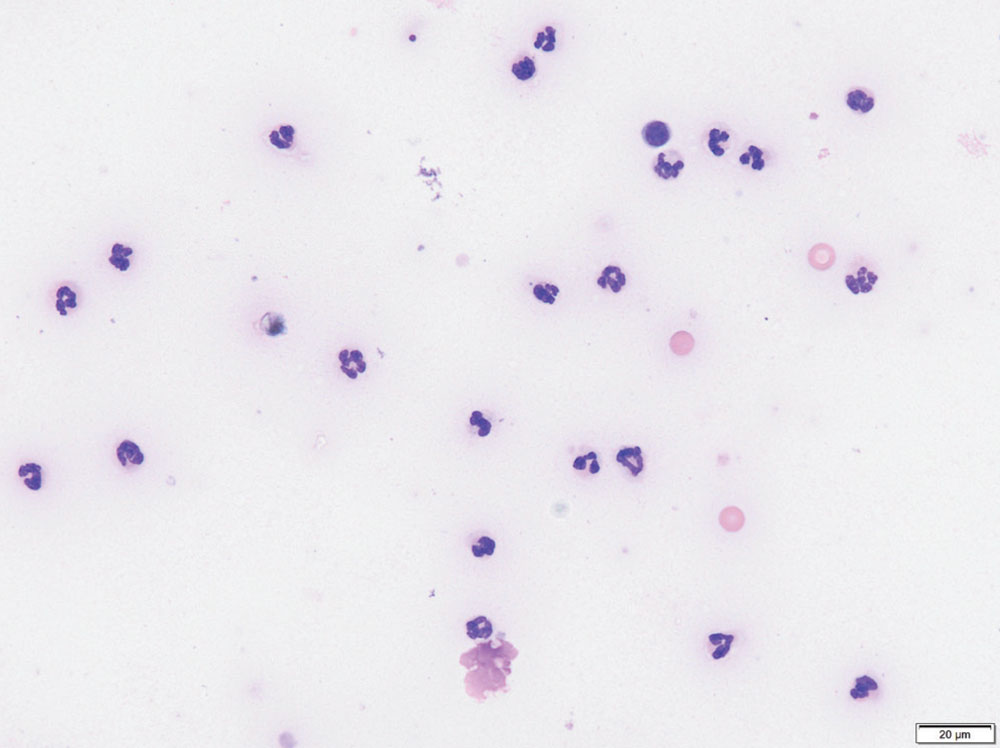
Figure 1: Cytology of joint fluid from a dog with IMPA. Non-degenerate neutrophils are the predominant cell type. Photo: Laureen Peters.
Additional diagnostics
Additional diagnostics may be appropriate in certain cases. Dogs presenting with clinical signs suggestive of other auto-immune problems, such as lesions on mucocutaneous junctions, should have an antinuclear antibody (ANA) test performed to screen for systemic lupus erythematosus.1 Cerebrospinal fluid analysis should be considered in dogs with neck or spinal pain, which could suggest concurrent steroid-responsive meningitis-arteritis. Measuring serum rheumatoid factor can be considered in dogs where erosive disease is suspected, but this test has limited sensitivity and specificity for diagnosing erosive IMPA.1
TREATMENT
Primary non-erosive IMPA
Immunosuppressive medications are indicated to treat primary immune-mediated polyarthritis.1 However, such medications are contraindicated in some of the differential diagnoses for IMPA, such as septic arthritis, and in many cases of secondary IMPA, for example where a vector-borne infection has been confirmed. It is, therefore, important that immunosuppressive therapy is not initiated until a diagnosis of IMPA has been confirmed cytologically and until secondary causes of IMPA have been ruled out.
Supportive care
Because it is usually not advisable to initiate immunosuppressive therapy immediately, for the reasons outlined above, analgesia is necessary in the short-term. Non-steroidal anti-inflammatory medications (NSAIDs) should be avoided when imminent initiation of corticosteroid therapy is anticipated, due to the risk of gastrointestinal ulceration or perforation when these medications are administered contemporaneously. If NSAIDs are used, a minimum washout period of seven days between stopping NSAIDs and starting corticosteroid therapy has been suggested.1 More appropriate analgesic options that can be used in patients with suspected IMPA include opioids (for example, intravenous methadone or a fentanyl patch), gabapentin, paracetamol or amantadine. Some dogs with IMPA can be systemically unwell, and additional medications or interventions may be indicated to manage their clinical signs, for example anti-emetics if nausea is present or intravenous fluid therapy if dehydration is detected.
Immunosuppressive medications
Glucocorticoids, especially prednisolone, are commonly used immunosuppressive medications to treat IMPA.1 Response is generally rapid, and it is common for clinical signs like joint effusion, pyrexia and joint pain to have completely resolved, or at least markedly improved, within 24-48 hours of starting treatment. It is important that the initial dose of prednisolone administered is an immunosuppressive dose; 2mg/kg/day PO SID is suggested as a starting dose in dogs weighing under 20kg. Because mg/kg dosing of prednisolone in dogs >20kg can result in those dogs receiving a relative overdose, an alternative dose of 40mg/m2 is suggested in those patients.31 SID dosing of prednisolone has been shown to have a lower incidence of adverse effects when compared to BID dosing.32 The dose of prednisolone should be reduced by approximately 25% every three to four weeks, assuming the dog remains in clinical remission. Repeating arthrocentesis would be ideal to confirm disease remission prior to tapering prednisolone, however performing arthrocentesis while dogs are on immunosuppressive therapy may increase the risk of iatrogenic septic arthritis. The author therefore does not advocate routinely repeating arthrocentesis. Instead, physical examination findings indicative of remission (absence of joint effusion, joint pain and pyrexia) should be used to decide whether or not tapering prednisolone is appropriate. Measuring serial C-reactive protein can also be used to determine disease remission in cases that are challenging to control.33,34 A second immunosuppressive agent can be added to the treatment protocol in dogs whose disease cannot be controlled with prednisolone alone or may be used to facilitate more rapid tapering of prednisolone in dogs who experience profound side effects of corticosteroid therapy. The most common second-agent immunosuppressive medications used to manage IMPA are listed in Table 1. It is suggested to continue the second agent immunosuppressive until one to two months after discontinuation of the tapering prednisolone course. Leflunomide appears to be an efficacious alternative single-agent option to prednisolone, and the use of this medication alone can be considered in dogs where long-term corticosteroid therapy is contraindicated due to concurrent diseases like diabetes mellitus.35 Dogs on long-term immunosuppressive therapy must be monitored for adverse effects of the medications. A complete blood count (and potentially a serum biochemistry depending on the immunosuppressive drugs used) should be checked two weeks after starting immunosuppressive therapy and thereafter every one to two months until immunosuppressive therapy is discontinued. Intermittent urinalysis and urine culture is also advised to screen for urinary tract infection while on these medications.
Secondary non-erosive IMPA
The primary focus when addressing secondary IMPA should be to treat the underlying disease. This may include treating an underlying neoplasm, treating a vectorborne disease with antimicrobial therapy or controlling gastrointestinal disease. If secondary IMPA has been triggered by medications or vaccination, signs may spontaneously resolve without immunosuppressive therapy once sufficient time has elapsed since exposure to the immune stimulus.14 In the event that clinical signs persist even when the underlying disease triggering IMPA has been controlled, immunosuppressive therapy is then indicated.
Erosive IMPA
As in non-erosive disease, immunosuppressive medications and analgesia are used to treat erosive IMPA. While monotherapy with corticosteroids is considered appropriate for management of dogs with non-erosive IMPA, it is contraindicated in erosive disease; in erosive disease, corticosteroid monotherapy is unlikely to be efficacious and may actually exacerbate damage to articular cartilage.6,36 Erosive IMPA should be managed with immunosuppressive doses of prednisolone in addition to a second immunosuppressive agent (as described in Table 1). Tapering of immunosuppressive agents is performed, as described above for non-erosive disease, but it is usually necessary to taper the medications more slowly, and it is rarely possible to completely discontinue immunosuppressive therapy in these cases.10 Treatment is less likely to be effective if significant damage to subchondral bone has already occurred. Dogs with erosive IMPA typically require lifelong analgesia and immunosuppressive therapy. Physiotherapy or surgical arthrodesis can be considered in some cases.37
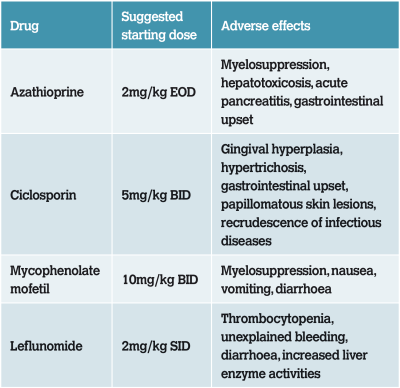
Table 1: Immunosuppressive medications commonly used alongside prednisolone to treat primary IMPA.
Prognosis
The prognosis of dogs with non-erosive IMPA depends on the underlying cause, but in general prognosis is good, with most dogs responding well to corticosteroid monotherapy or combination immunosuppressive drug therapy. Dogs with erosive IMPA will require lifelong therapy and the response to treatment and long-term prognosis are generally considered poor.1
Conclusion
IMPA is a disease with many different clinical presentations, and therefore should be considered as a differential diagnosis even in dogs without obvious joint effusion or joint pain. A comprehensive diagnostic approach is necessary to distinguish IMPA from other joint diseases, to distinguish primary IMPA from secondary IMPA and to identify if the disease is erosive or non-erosive.
-
Stone M. Textbook of Veterinary Internal Medicine. 8th edition. St Louis: Saunders; 2017. Chapter 203. Immune-mediated polyarthritis and other polyarthritidies; p. 861-866.
-
Jacques D, Cauzinille L, Bouvy B, et al. A retrospective study of 40 dogs with polyarthritis. Veterinary Surgery 2002;27:51-59.
-
Dunn K, Dunn J. Diagnostic investigations in 101 dogs with pyrexia of unknown origin. Journal of Small Animal Practice 1998;39:574-580.
-
Stull J, Evason M, Anthony C, et al. Canine immune-mediated polyarthritis: clinical and laboratory findings in 83 cases in western Canada (1991-2001). The Canadian Veterinary Journal 2008;49:1195-1203.
-
Johnson K, Mackin A. Canine immune-mediated polyarthritis part 1: pathophysiology. Journal of the America Animal Hospital Association 2012;48:12-17.
-
Rondeau M, Walton R, Bisset S, et al. Suppurative, nonseptic polyarthropathy in dogs. Journal of Veterinary Internal Medicine 2005l19:654-662.
-
Clements D, Gear R, Tattersall J, et al. Type 1 immune-mediated polyarthritis in dogs: 39 cases (1997-2002). Journal of the American Veterinary Medical Association 2004;224:1323-1327.
-
Sbrana S, Marchetti V, Mancianti F, et al. Retrospective study of 14 cases of canine arthritis secondary to Leishmania infection. Journal of Small Animal practice 2015;55:309-313.
-
Gear R, Bacon N, Langley-Hobbs S, et al. Panniculitis, polyarthritis and osteomyelitis associated with pancreatic neoplasia in two dogs. Journal of Small Animal Practice 2006;47:400-404.
-
Taylor S. Small animal internal medicine. 4th edition. St Louis: Elsevier; 2009. Chapter 10. Joint disorders; p.1119-1141.
-
Giger U, Werner L, Millichamp N, et al. Sulfadiazine-induced allergy in six Doberman pinschers. Journal of the American Veterinary Medical Association 1985;186:479-84.
-
Bennett D. Immune-based non-erosive inflammatory joint disease of the dog. 3. Canine idiopathic polyarthritis. Journal of Small Animal Practice 1987;28:909-928.
-
Cribb A, Spielberg S. An in vitro investigation of predisposition to sulphonamide idiosyncratic toxicity in dogs. Veterinary Research Communications 1990;14:241-252.
-
Kohn B, Garner M, Lübke S, et al. Polyarthritis following vaccination in four dogs. Veterinary and Comparative Orthopaedics and Traumatology 2003;16:6-10.
-
Dodds W. Vaccination protocols for dogs predisposed to vaccine reactions. Journal of the American Animal Hospital Association 2001;37:211-214.
-
Marks S, Henry C. Kirks current veterinary therapy XIII: small animal practice. 13th edition. Philadelphia: Saunders; 2000. Diagnosis and treatment of systemic lupus erythematosus; p.514-516.
-
Stone M. Textbook of Veterinary Internal Medicine. 8th edition. St Louis: Saunders; 2017. Chapter 205. Systemic lupus erythematosus; p.873-876.
-
Berent A, Cerundolo R. Systemic lupus erythematosus. Standards of Care 2005;7:7-12.
-
Dougherty S, Center S, Shaw E, et al. Juvenile-onset polyarthritis syndrome in Akitas. Journal of the American Veterinary Medical Association 1991;198:849-856.
-
Rivas A, Tintle L, Meyers-Wallen V, et al. Inheritance of renal amyloidosis in Chinese Shar-pei dogs. Journal of Heredity 1993;84:438-442.
-
Rivas A, Tintle L, Kimball E, et al. A canine febrile disorder associated with elevated interleukin-6. Clinical Immunology and Immunopathology 1992;64:36-45.
-
May C, Hammill J, Bennett D. Chinese shar pei fever syndrome: a preliminary report. Veterinary Record 1992;131:586-587.
-
Tellier L. Immune-mediated vasculitis in a shar-pei with swollen hock syndrome. Canadian Veterinary Journal 2001;42:137-139.
-
Carr A, Michels G. Identifying noninfectious erosive arthritis in dogs and cats. Veterinary Medicine 1997;92:804-810.
-
Woodard C, Riser W, Bloomberg M, et al. Erosive polyarthritis in two greyhounds. Journal of the American Veterinary Medical Association 1991;198:873-876.
-
Black V., Whitworth F, Adamantos S. Pyrexia in juvenile dogs: a review of 140 referred cases. Journal of Small Animal Practice 2019;60:116-120.
-
Shaughnessy M, Sample S, Abicht C, et al. Clinical features and pathological joint changes in dogs with erosive immune-mediated polyarthritis: 13 cases (2004–2012). Journal of the American Veterinary Medical Association 2016;249:1156-1164.
-
Innes J. Veterinary Surgery. St Louis: Saunders; 2012. Arthritis; p. 1078-1111.
-
MacWilliams P, Friedrichs K. Laboratory evaluation and interpretation of synovial fluid. Veterinary Clinics of North America: Small Animal Practice 2003;33:153-178.
-
Johnson K, Mackin A. Canine immune-mediated polyarthritis: part 3: diagnosis and treatment. Journal of the American Hospital Association 2012;48:71-82.
-
Nam A, Kim S, Jeong J, et al. Comparison of body surface area-based and weight-based dosing format for oral prednisolone administration in small and large-breed dogs. Polish Journal of Veterinary Sciences 2017;20:611-613.
-
Swann J, Szladovits B, Threlfall A, et al. Randomised controlled trial of fractionated and unfractionated prednisolone regimens for dogs with immune-mediated haemolytic anaemia. Veterinary Record 2019;184:771.
-
Kjelgarrd-Hansen M, Jensen A, Houser G, et al. Use of serum C-reactive protein as an early marker of inflammatory activity in canine type II immune-mediated polyarthritis: case report. Acta Veterinaria Scandinavica 2006;48:9.
-
Ohno K, Yokoyama Y, Nakashima K, et al. C-reactive protein concentration in canine idiopathic polyarthritis. Journal of Veterinary Medical Science 2006;68:1275-1279.
-
Colopy S, Baker T, Muir P. Efficacy of leflunomide for treatment of immune-mediated polyarthritis in dogs: 14 cases (2006-2008). Journal of the American Veterinary Medical Association 2010;236:312-318.
-
Hossain M, Park J, Choi S, et al. Dexamethasone induces apoptosis in proliferative canine tendon cells and chondrocytes. Veterinary and Comparative Orthopaedics and Traumatology 2008;21:337-342.
-
Ralphs S, Beale B, Whitney W, et al. Idiopathic erosive polyarthritis in six dogs (description of the disease and treatment with bilateral pancarpal arthrodesis). Veterinary and Comparative Orthopaedic Traumatology 200;13:191-196.
1. Non-erosive IMPA generally occurs as a result of what type of hypersensitivity reaction?
A. Type I
B. Type II
C. Type III
D. Type IV
2. Which breed is affected by a distinct type of IMPA that represents a form of familial amyloidosis?
A. Beagle
B. Shar Pei
C. Jack Russell Terrier
D. Greyhound
3. What is the predominant cell type in normal synovial fluid?
A. Non-degenerate neutrophil
B. Degenerate neutrophil
C. Mononuclear cell
D. Epithelial cell
4. Bacterial culture is positive in what percentage of cases of septic arthritis?
A. 10-20%
B. 40-50%
C. 70-80%
D. 90-100%
5. The anti-nuclear antibody (ANA) test is used to diagnose what condition?
A. Systemic lupus erythematosus (SLE)
B. Non-erosive immune-mediated polyarthritis
C. Steroid-responsive meningitis-arteritis (SRMA)
D. Erosive immune-mediated polyarthritis
Answers: 1C; 2B; 3C; 4B; 5A.















